Do you feel flat regularly?
Do you feel flat regularly?
Are you having problems sleeping?
Have you noticed changes in your libido?
Do you have hypertension but there’s no family history?
Do you negotiate feelings of depression and sadness on a daily basis?
Do you get out of bed in the morning with a spring in your step? Or do you drag yourself out of bed?
Have you noticed that you don’t really ‘wake up’ for the day until around 10-11am?
Have you observed having a coffee at a set time because ‘it gets you through the afternoon’?
Do you regularly have a late afternoon stimulant hit of caffeine/chocolate/sugar or sugary products/other?
Are you tired of being tired all the time?
Have you been using the oral contraceptive pill for a long time?
Do you find that you can’t muster the energy to do the activities you really enjoy?
Have you had enough, and need some possible answers?
Then read on……….!
Adrenal fatigue was first described by Thomas Addison (1793-1860) but the term ‘Adrenal Fatigue’ was coined in the 1990’s and one of the first names attributed to recognising (and later writing about it) was Dr James L Wilson. The condition has for a long time evaded medical acceptance because the diagnosis of ‘adrenal fatigue’ didn’t sit nicely within the current paradigm. You either had Addison’s Disease or Cushing’s Disease – both, at each extreme of the adrenal continuum with a whole spectrum of possible signs and symptoms in between. In modern clinical practice, the majority of people have some degree of adrenal insufficiency, and unfortunately, my clinic is no different.
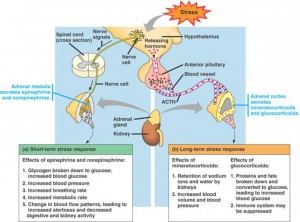
Adrenals are two pyramid like glands that sit on top of each kidney, and are part of the endocrine system because they secrete messenger hormones/neurotransmitters. They consist of 4 layers encased in a capsule. The anatomy looks like this –
- Medulla – innermost layer > produces adrenalin and noradrenalin
- Cortex – outer most layer, has 3 sub-layers –
- Zona reticularis – produces sex hormones
- Zona fasciculata – produces glucocorticoids to regulate blood glucose levels
- Zona glomerulosa – produce mineralocorticoids to regulate electrolytes/minerals
Being part of the endocrine system, they interact with other glands such as the thyroid, parathyroid, gonads, hypothalamus, pituitary, pineal, pancreas and thymus. They interact using a complex biofeedback system reliant on conducting surveillance on levels of hormones/neurotransmitters in the blood and communicating with each other using primarily the chemical messengers we know as hormones or neurotransmitters.
The ‘fatigue’ part of adrenal fatigue occurs where the adrenal glands can no longer continue to produce all the hormones they need to, usually as a result of prolonged stress.
Causes of adrenal fatigue –
 Any number of factors can cause adrenal fatigue, just take a look at the diagram. However, the key to understanding adrenal fatigue are the concepts of stress and cortisol production – the master stress hormone. When I ask people in clinic to rate their stress, invariably I get low ratings. But when I explain that the body has one primary mechanism in its reaction to stress, their ratings change, but also because their definition of stress is challenged.
Any number of factors can cause adrenal fatigue, just take a look at the diagram. However, the key to understanding adrenal fatigue are the concepts of stress and cortisol production – the master stress hormone. When I ask people in clinic to rate their stress, invariably I get low ratings. But when I explain that the body has one primary mechanism in its reaction to stress, their ratings change, but also because their definition of stress is challenged.
A little bit of stress is actually quite necessary, however stress, whether physical, emotional, psychological, mental, spiritual, financial, environmental, etc. has one main effect in the initial phase – to increase the activity of your sympathetic nervous system (SNS) and increase your production of adrenalin and noradrenalin (neurotransmitters), otherwise known as the Fight or Flight Response. One of the many possible reasons why people find that sleep is affected in this phase is because adrenalin opposes the production of melatonin (the sleep hormone that helps you sleep). Other hormones such as cortisol are also produced in this phase. However, if you are constantly or chronically in a heightened stress response state , also known as SNS Dominance, production of adrenalin and noradrenalin decreases and cortisol increases and stays high. At this point symptoms such as anxiety, agitation, poor sleep, poor digestion, inability to lose weight especially around the mid-section, or even panic can be experienced.
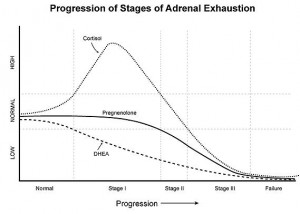
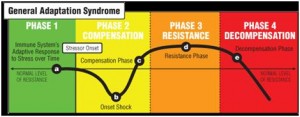 Eventually (months in some people, years in others) production of these hormones reduces and you experience many more of the symptoms described in the table below, eventually leading to burnout and ultimately adrenal fatigue, where the adrenal glands can no longer continue to produce all the hormones they need to. This progression is known as the General Adaptation Syndrome (GAS, Hans Selye) and can be shown like this (please note that the timing of each phase is very unique to each individual).
Eventually (months in some people, years in others) production of these hormones reduces and you experience many more of the symptoms described in the table below, eventually leading to burnout and ultimately adrenal fatigue, where the adrenal glands can no longer continue to produce all the hormones they need to. This progression is known as the General Adaptation Syndrome (GAS, Hans Selye) and can be shown like this (please note that the timing of each phase is very unique to each individual).
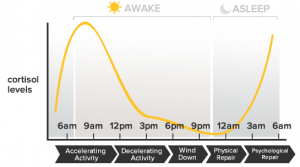 Importantly, cortisol production has a daily rhythm (also known as the diurnal cortisol pattern, DCP). So when your body continues to produce cortisol for extended periods of time as a consequence of an overactive stress response, the production of other hormones such as your sex hormones (androgens, pregnenolone, DHEA) and the hormones that regulate mineral/electrolyte balance (mineralocorticoids, aldosterone) in the body suffer too. See next diagram.
Importantly, cortisol production has a daily rhythm (also known as the diurnal cortisol pattern, DCP). So when your body continues to produce cortisol for extended periods of time as a consequence of an overactive stress response, the production of other hormones such as your sex hormones (androgens, pregnenolone, DHEA) and the hormones that regulate mineral/electrolyte balance (mineralocorticoids, aldosterone) in the body suffer too. See next diagram.
 Now, cortisol is not all bad. It is a necessary hormone involved in controlling inflammatory reactions and in particular in managing some white blood cells (amongst others) that if left unmanaged could result in more complicated inflammatory responses. However, it is the prolonged release of cortisol at consistently high levels that results in symptoms such as decreased immunity, tendency to bruise easily, anxiety, irritability, skin eruptions, poor or compromised digestion, etc.. BUT, the crucial point is that the DCP can be measured over the course of the day (discussed below), and this has implications for many health complaints including people suffering from insulin resistance/metabolic syndrome, people who have tried to lose weight repeatedly without ever achieving satisfactory results only to find their weight always comes back, suspected thyroid disorders, poor sexual function, blood pressure management, amongst others.
Now, cortisol is not all bad. It is a necessary hormone involved in controlling inflammatory reactions and in particular in managing some white blood cells (amongst others) that if left unmanaged could result in more complicated inflammatory responses. However, it is the prolonged release of cortisol at consistently high levels that results in symptoms such as decreased immunity, tendency to bruise easily, anxiety, irritability, skin eruptions, poor or compromised digestion, etc.. BUT, the crucial point is that the DCP can be measured over the course of the day (discussed below), and this has implications for many health complaints including people suffering from insulin resistance/metabolic syndrome, people who have tried to lose weight repeatedly without ever achieving satisfactory results only to find their weight always comes back, suspected thyroid disorders, poor sexual function, blood pressure management, amongst others.
Note – One cortisol test result measurement at a point in time does not accurately convey what is happening or ‘trending’ in your body throughout the course of your ‘stressful’ day that would enable correct identification of management strategy. Please see below for how to test.
Here’s how it works…
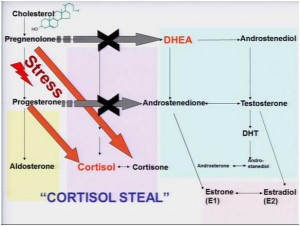 Cortisol is the metabolic end product of a series of biochemical and enzymatic reactions that convert cholesterol (produced in the liver – yes that’s right, our liver produces nearly 85% of the total cholesterol our body needs). Cortisol is the master stress hormone but is also released in times of low blood glucose concentrations, for example, when the body undergoes a fasting stated at night while sleeping. In the pathway from cholesterol to cortisol, two products that are produced in the sequence are pregnenolone and progesterone. If all the pregnenolone and progesterone are diverted to produce cortisol, there is very little, if any, product to be used to convert to either DHEA to make sex hormones, or Aldosterone (the hormone that regulates mineral/electrolyte balance). This is known as the Cortisol Steal or the Pregnenolone Steal.
Cortisol is the metabolic end product of a series of biochemical and enzymatic reactions that convert cholesterol (produced in the liver – yes that’s right, our liver produces nearly 85% of the total cholesterol our body needs). Cortisol is the master stress hormone but is also released in times of low blood glucose concentrations, for example, when the body undergoes a fasting stated at night while sleeping. In the pathway from cholesterol to cortisol, two products that are produced in the sequence are pregnenolone and progesterone. If all the pregnenolone and progesterone are diverted to produce cortisol, there is very little, if any, product to be used to convert to either DHEA to make sex hormones, or Aldosterone (the hormone that regulates mineral/electrolyte balance). This is known as the Cortisol Steal or the Pregnenolone Steal.
Hence, the relationship of chronic stress with high cortisol production, low sex hormone production, low aldosterone, poor blood sugar management. The easy way to remember the relevance of the adrenal glands and the important functions they maintain can be depicted as follows –
- Sugar (glucocorticoids, cortisol)
- Salt (mineralocorticoids, aldosterone)
- Sex (androgens, sex hormones)
What are examples of conditions and signs/symptoms of adrenal fatigue?
The following table summarises many of the diagnosed conditions and preceding signs/symptoms that can be associated with adrenal fatigue.
Conditions |
Signs/Symptoms |
|---|---|
| Fibromyalgia
Alcoholism Ischaemic Heart Disease Hypoglycemia or hyperglycemia Rheumatoid Arthritis Chronic & recurrent respiratory infections Alopecia Chronic Fatigue Syndrome (CFS) Addictions Autoimmune disease Depression PMS & hormone disorders Menopause, e.g. early onset Allergies Skin conditions – eczema, psoriasis, fungal infections Hypertension or Hypotension Metabolic Syndrome Renal disease Hyponatremia (low sodium) Hyperkalemia (high potassium) Thyroid disorders IBS and digestive issues Post Natal Depression Pre-diabetes or Type 2 Diabetes Prostate Disorder Liver Dysfunction Erectile dysfunction |
Poor or decreased sex drive/libido
Constant fatigue – not relieved by sleep Craving salt or salty foods Energy conservation – increased effort to do everyday tasks Poor or declining memory Anxiety and/or irritability Increased recovery time from illness, injury or trauma Orthostatic hypertension Decreased tolerance Decreased productivity Poor quality of life Don’t really wake up till 10am, afternoon low between 3-4pm, feel better after evening meal (usually 6pm) Fat deposits especially around the face, upper back, between the shoulders and mid-section (visceral adiposity) Weight gain or inability to lose weight adequately ‘Wired’ yet ‘tired Poor sleep Hyperpigmentation of the skin Increased pain perception Decreased melatonin production Electrolyte imbalances Early signs of ageing Poor digestion Bone and muscle loss Sugar cravings Poor stress management Mood or behavioural changes Insulin resistance Cortisol resistance Facial hair growth in women Joint aches and pains Fluid retention Heavy metal exposures |
How do I test? What do I test?
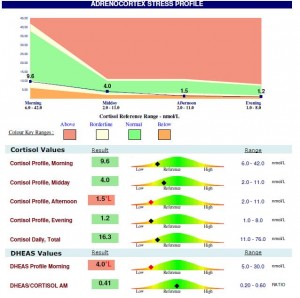
Fortunately, there is a reliable, non-intrusive clinical method of testing for adrenal hormones using saliva. The attached diagram is a sample report of a person that is unable to lose weight because of long term chronic stress and the impact on the adrenals. This diagram describes the type of person whose adrenals are struggling to produce adequate levels of hormones and if no intervention takes place, will ultimately end in burnout.
In clinical practice, additional tests may be necessary such as thyroid studies, iron studies, melatonin, vitamin D status, zinc/copper ratio, neurotransmitter status, amongst others, but this is extremely personalised on a case by case basis depending on presenting complaints, case history, and desired health outcomes. Importantly, it is advised that you see a qualified healthcare practitioner if you suspect you may have adrenal fatigue or have been suffering from any of the above mentioned signs/symptoms with no adequate resolution.
What can YOU do NOW?
The first thing you can do is assess lifestyle choices.
- Are you going to sleep around 9.30-10pm when the adrenal glands should be decreasing in activity to allow you to produce melatonin?
- Do you need sleep hygiene advice?
- Are you drinking alcohol every Friday and Saturday night? Or every night?
- Are you eating a whole food, preferably organic, diet that is low in sugar and refined carbohydrates?
- Are you drinking enough water?
- Are you exercising regularly (3-4 times a week aerobically)?
- Are you self-medicating without identifying the cause?
- Do you have a positive support network? Or do some of your family/friends ‘stress you out’? If so, you may want to review the health of that relationship!
- Are you trying to do too much?
- Parenting duties
- School runs
- Working additional hours
- A punishing exercise routine
- Running a household
- Starting or running a business
- Work in a high-pressure executive role
- etc., etc.
- Do you regularly plan in some rest & vital relaxation time?
- Are you being nurtured in ways that are right for you?
Some key nutrients that help support adrenal glands are:
- Vitamin C + co-factors – almost 4g of the bodys’ total 5g of vitamin C are used by the adrenal glands on a daily basis, mainly in the production of cortisol!
- Magnesium – is it the right form of magnesium? (if you’re not sure you may want to check my article on How to Choose the Right Multivitamin)
- Vitamin B’s – in particular B5 and B6
- Iodine
- Selenium
- Zinc
- Tyrosine
- Turmeric
- Probiotics
There are also some herbal medicines to consider for adrenal support and restoration. Rehmannia and Licorice are the two best known.
In addition, there are herbal medicines that have adaptogenic actions, i.e. they modulate or adapt the body’s response to stress. Some good examples are Siberian Ginseng, Withania, Korean Ginseng, Rhodiola, Gotu Kola, and Schisandra. These were traditionally used in Russian athletes.
The last thing that you can do, is get tested. Once you know the facts, it’s much easier to manage and then monitor changes and results.
Finally, depending on the level of adrenal depletion, therapeutically timed doses of some of these nutrients may be required along with high quality herbal medicines that have been standardised for active ingredients – as not all products are created equal! It’s also important to note that while these supportive measures greatly assist, they should be used in conjunction with a plan to address underlying cause(s), which ultimately has the best chance for delivering long term, quality health outcomes. Further, any prescribed medications may have interactions with undertaking comprehensive nutritional adrenal support therapy, and a qualified professional can help you navigate this in a safe and healthy way.
Special Note – If you are on glucocorticosteroid medication, or ANY medication, you must NOT abruptly stop using the medication as there can be serious health consequences. Always seek professional medical advice.
If you thought this article was helpful, don’t forget to like on Facebook or share with your friends.
___________________________________________________
Sarina completed her Bachelor’s degree with a special interest in Neuroscience and specialises in reverse engineering your symptoms to identify and address underlying cause(s). She has additional special interests in Functional Medicine since training and practising in the USA as a clinical nutritionist & herbalist (2003-2007). In clinic, specialist laboratories are used that have Australian accreditation.
Resources and References:
Dr James L Wilson, Adrenal Fatigue: the 21st century syndrome, https://www.adrenalfatigue.org/
http://cortisolconnection.com/
http://www.drfranklipman.com/adaptogens-natures-miracle-anti-stress-and-fatigue-fighters/
http://bodyecology.com/articles/adaptogens_how_to_eliminate_stress.php
——
Adrenal Insufficiency, 2013 – http://www.ncbi.nlm.nih.gov/pubmed/25905309
An overview on ashwagandha: a Rasayana (rejuvenator) of Ayurveda, 2011 – http://www.ncbi.nlm.nih.gov/pubmed/22754076
Assessing stress reactivity indexed via salivary cortisol in preschool-aged children, 2011 – http://www.ncbi.nlm.nih.gov/pubmed/21388745
Breakthrough Solutions in Herbal Medicine Adaptogenic Formulas: The Way to Vitality.” Townsend Letter. January 2007, www.townsendletter.com
Defensive coping and renovascular disease risk – Adrenal fatigue in a cohort of Africans and Caucasians: The SABPA study, 2015 – http://www.ncbi.nlm.nih.gov/pubmed/25911265
Inhaled corticosteroids and secondary adrenal insufficiency, 2014 – http://www.ncbi.nlm.nih.gov/pubmed/25674179
Panax ginseng, Rhodiola rosea and Schisandra chinensis, 2012 – http://www.ncbi.nlm.nih.gov/pubmed/22039930
Plant adaptogens, 1994 – http://www.ncbi.nlm.nih.gov/pubmed/23195818
Protective effects of Andrographis paniculata extract and pure andrographolide against chronic stress-triggered pathologies in rats, 2014 – http://www.ncbi.nlm.nih.gov/pubmed/25035059
Salivary cortisol as an indicator of physological stress in children and adults; a systematic review, 2014 – http://www.ncbi.nlm.nih.gov/pubmed/24951973
Salivary cortisol levels as a biological marker of stress reaction, 2013 – http://www.ncbi.nlm.nih.gov/pubmed/24601177
The gut microbiome and the brain – http://www.ncbi.nlm.nih.gov/pubmed/25402818
Graphics –
http://corporatefunrun.com/are-your-adrenals-in-a-knot/
http://www.nursebuff.com/nursing-mnemonics-and-acronyms-respiratory-endocrine-and-nervous-systems/
http://www.proprofs.com/flashcards/story.php?title=bio-lecture-4-page-12411-lecture-pt-1